
Key takeaway / Summary of topic answer
For women with a history of ectopic pregnancy, undergoing a fertility assessment before planning another pregnancy is a crucial step to reduce risks and improve the chances of a successful outcome—whether through natural conception or IVF. The evaluation should comprehensively assess the health of the uterus, fallopian tubes, and ovaries, as well as identify any inflammation or adhesions that may affect embryo implantation. Early consultation and treatment planning with a reproductive medicine specialist can help prevent recurrent ectopic pregnancy and support a safer, more confident pregnancy journey.
Planning a pregnancy after an ectopic pregnancy requires more than simply waiting for physical recovery. It is a phase that calls for a deeper understanding of one’s reproductive health, courage to move forward, and accurate medical information. Even after treatment is completed, the reproductive system often needs a comprehensive evaluation to ensure that the next pregnancy can progress safely and with the lowest possible risk of recurrence.
Many women can conceive again after an ectopic pregnancy, whether naturally or through assisted reproductive technologies. The key lies in understanding the true condition of the body and choosing the most appropriate path forward before attempting conception. This proactive approach helps reduce the risk of recurrent ectopic pregnancy and supports a smoother, more confident journey toward a healthy pregnancy.
Symptoms and Complications of Ectopic Pregnancy
An ectopic pregnancy occurs when an embryo implants outside the uterine cavity, most commonly in the fallopian tube, although implantation may also occur in the cervix or abdominal cavity. The fallopian tube is the most frequent site because it is the pathway the egg travels before reaching the uterus.
Treatment depends largely on the severity of the condition and may include medication, conservative surgery that preserves the tube, or fallopian tube surgery to remove the affected tube. Even after surgical treatment, pregnancy is still possible, as the ovaries continue to function normally and the remaining fallopian tube can often capture eggs released from either ovary.
Early Signs of Ectopic Pregnancy
In the early stage, symptoms may resemble those of a normal pregnancy, making the condition difficult to detect, such as:
- Lower abdominal pain or unilateral pelvic discomfort
- Abnormal vaginal bleeding, often dark or spotting
- Dizziness, fatigue, or nausea
- Rising hCG levels that increase more slowly than in a normal pregnancy
Severe Symptoms Requiring Immediate Medical Attention
If the embryo continues to grow in an inappropriate location, the fallopian tube may rupture, causing severe internal bleeding and becoming life-threatening. Warning signs include:
- Suddenly, severe abdominal pain
- Pain radiating to the shoulder or back
- Fainting or loss of consciousness due to internal bleeding
Long-Term Effects After Ectopic Pregnancy
Even with timely emergency treatment, ectopic pregnancy may leave long-term effects on reproductive health, including:
- Pelvic adhesions or scar tissue
- Partial or complete dysfunction of the fallopian tube
- Increased risk of recurrent ectopic pregnancy
- Emotional distress, anxiety, and reduced confidence when planning future pregnancies
These effects highlight why a thorough fertility assessment is essential before attempting to conceive again, helping protect both maternal and fetal health.
Have a history of ectopic pregnancy and planning to conceive? Get expert guidance at VFC Center
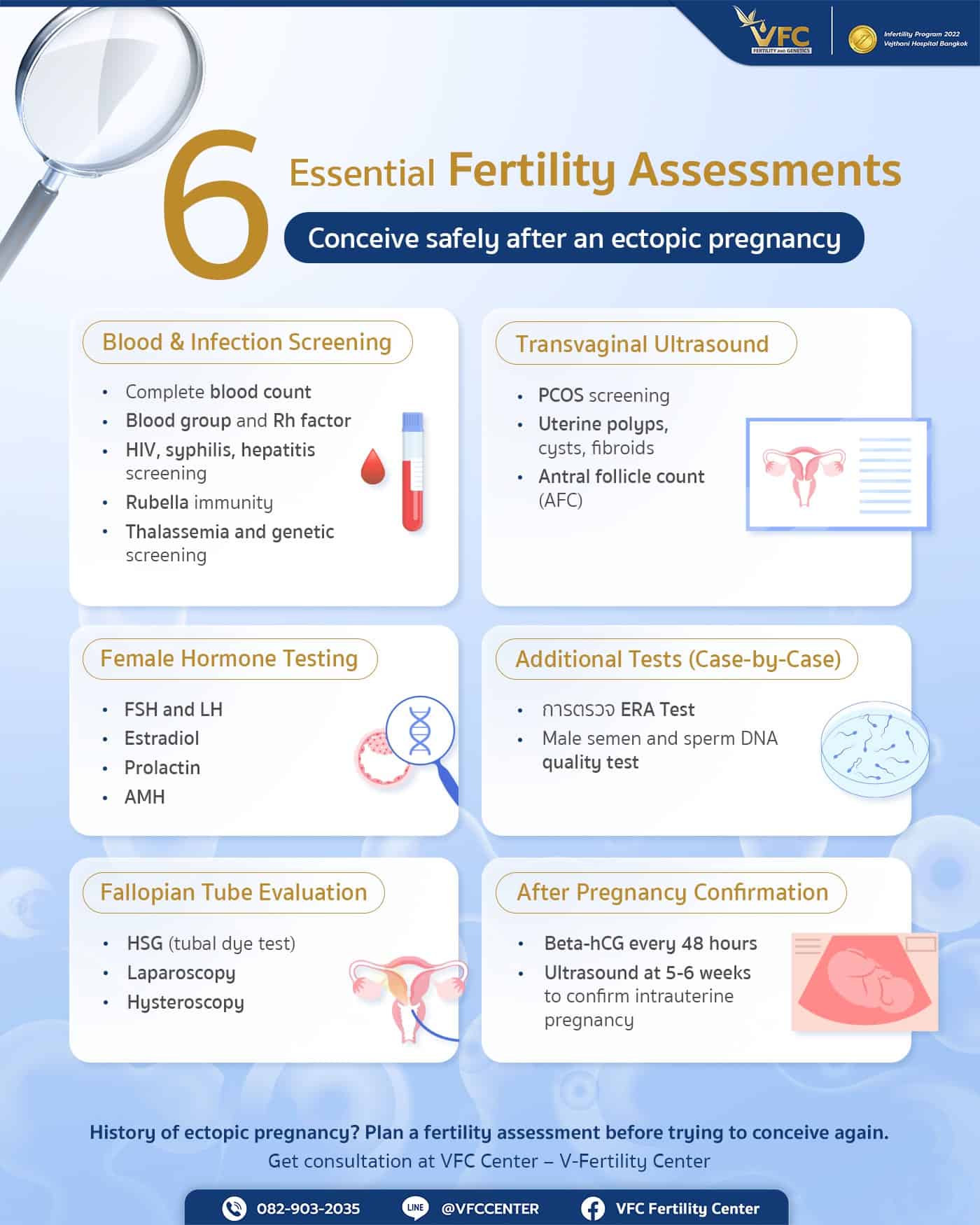
Fertility Assessment for Pregnancy Planning After Ectopic Pregnancy
Women with a history of ectopic pregnancy require a more detailed evaluation than those planning pregnancy for the first time. The goal is not only to achieve pregnancy but to ensure it occurs safely. Studies show a recurrence risk of approximately 10-15%, making comprehensive fertility assessment especially important.
Blood Tests and Infectious Disease Screening
Basic tests that evaluate overall health and reduce risks to both mother and baby include:
- Complete blood count
- Blood type and Rh factor
- Screening for HIV, syphilis, and hepatitis viruses
- Rubella immunity
- Thalassemia and other genetic disorder screening
Female Hormone Testing and Egg Quality Evaluation
Hormonal balance plays a critical role in ovulation and fertility. These tests are typically performed on days 2-3 of the menstrual cycle and include:
- FSH and LH to assess ovarian function
- Estradiol to evaluate hormonal balance
- Prolactin, as elevated levels may interfere with ovulation
- AMH to estimate remaining egg quantity and quality
Transvaginal Ultrasound Examination
This imaging test evaluates reproductive organs and includes:
- Screening for polycystic ovary syndrome (PCOS)
- Detecting endometrial polyp, ovarian cysts, or uterine fibroids that may interfere with implantation
- Assessing antral follicle count (AFC)
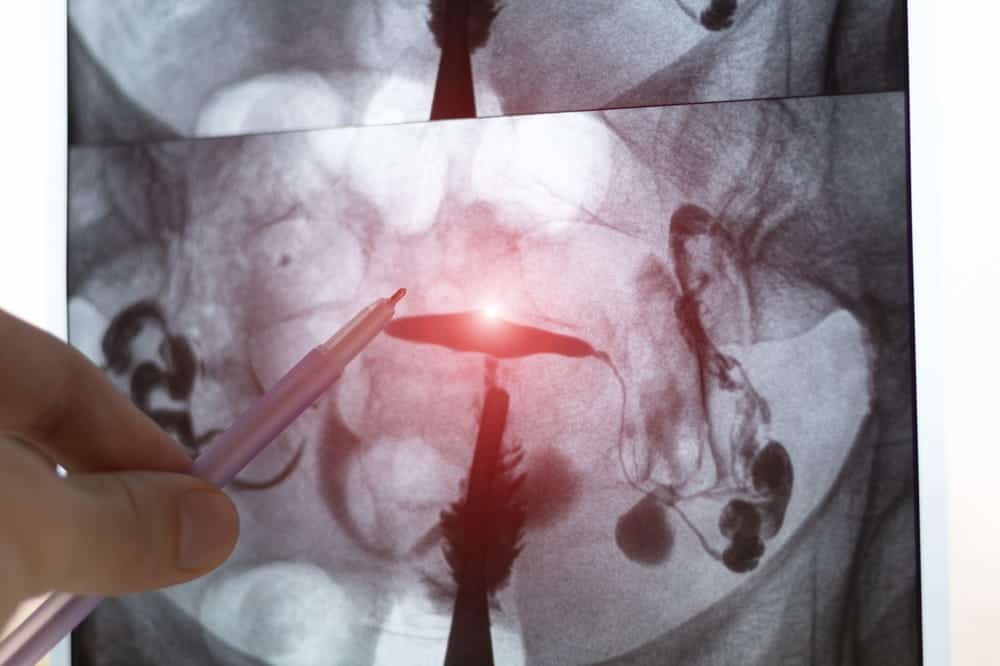
Evaluation of Fallopian Tubes and Uterine Cavity
Especially important for women with prior ectopic pregnancy, these tests help reduce recurrence risk:
- Hysterosalpingography (HSG) to assess whether the remaining fallopian tube is open
- Laparoscopy to directly evaluate adhesions or inflammation
- Hysteroscopy to identify uterine cavity abnormalities affecting implantation
Additional Tests in Selected Cases
Depending on individual health conditions and physician judgment, additional evaluations may include:
- ERA testing to assess endometrial receptivity in patients with repeated failed IVF cycles
- Semen analysis and sperm DNA quality testing for the male partner
Monitoring After Pregnancy Is Confirmed
Even after successful conception, women with a history of ectopic pregnancy should have serial Beta-hCG testing every 48 hours to ensure appropriate hormone rise, followed by a transvaginal ultrasound at 5-6 weeks of gestation to confirm that the pregnancy is located within the uterus.
Inquire about fertility assessment packages before pregnancy at VFC Center
How to Reduce the Risk of Ectopic Pregnancy From the First Pregnancy Plan
Although ectopic pregnancy cannot be prevented entirely, risk can be reduced with careful planning:
- Pre-pregnancy reproductive health screening: Allows early evaluation of the uterus, fallopian tubes, and ovaries to guide safe conception planning
- Prevent pelvic inflammatory disease (PID): Pelvic inflammatory infection can cause inflammation, narrowing, or scar tissue formation in the fallopian tubes and can be prevented through three key approaches.
- Practice safe sex to avoid sexually transmitted infections
- Seek treatment promptly for abnormal vaginal discharge or pelvic inflammation
- Avoid unnecessary vaginal douching
- Avoid behaviors that damage fallopian tube function: Nicotine impairs ciliary movement within the fallopian tubes, disrupting egg and embryo transport and increasing implantation risk outside the uterus
- Choose appropriate conception methods: When tubal risk is high, assisted reproductive technologies such as IVF may reduce reliance on the fallopian tubes and lower ectopic pregnancy risk
- Confirm pregnancy location early: Early Beta-hCG testing and transvaginal ultrasound at 5–6 weeks help confirm proper uterine implantation
A history of ectopic pregnancy does not mean the end of fertility. It means that future pregnancy planning requires deeper understanding, comprehensive fertility assessment, and early consultation with reproductive medicine specialists. Whether pursuing natural conception or assisted reproductive options such as IVF, personalized planning significantly improves safety and confidence.
Plan your fertility evaluation and pregnancy readiness with VFC Center (V Fertility Center). Our reproductive medicine specialists provide individualized care from the very beginning, helping you choose the safest path forward at a trusted fertility treatment center.
Article by Dr. Wanakan Singhasena
Contact or Book a Consultation:
VFC Center – V-Fertility Center
Hotline: 082-903-2035
LINE Official: @vfccenter
Frequently Asked Questions (FAQs)
What should I do if fallopian tube adhesions or abnormalities are found?
Consultation with a reproductive medicine specialist is recommended to consider IVF or other appropriate fertility treatments.
When should hCG blood testing be done after ectopic pregnancy history?
Testing is typically performed 10-14 days after implantation to confirm pregnancy and closely monitor hormone progression.
Can I conceive naturally after an ectopic pregnancy?
Natural conception is possible if the remaining fallopian tube functions well, but a full fertility assessment is advised for safety.
Does fallopian tube surgery affect long-term health?
While it may reduce natural conception rates, fallopian tube surgery does not pose long-term health risks.

OBSTETRICS AND GYNAECOLOGY-REPRODUCTIVE MEDICINE





No Comments
Sorry, the comment form is closed at this time.